Borges H, Dufau A, Paneri B, Woods AJ, Knotkova H, Bikson M. Updated Technique for Reliable, Easy, and Tolerated Transcranial Electrical Stimulation Including Transcranial Direct Current Stimulation. Journal of Visualized Experiments 2020. https://doi.org/10.3791/59204.
Esmaeilpour Z, Shereen AD, Ghobadi‐Azbari P, Datta A, Woods AJ, Ironside M, O’Shea J, Kirk U, Bikson M, Ekhtiari H. Methodology for tDCS integration with fMRI. Human Brain Mapping. 2019 Dec 24; Available from: http://dx.doi.org/10.1002/hbm.24908
Download PDF published in Human Brain Mapping — DOI
Abstract
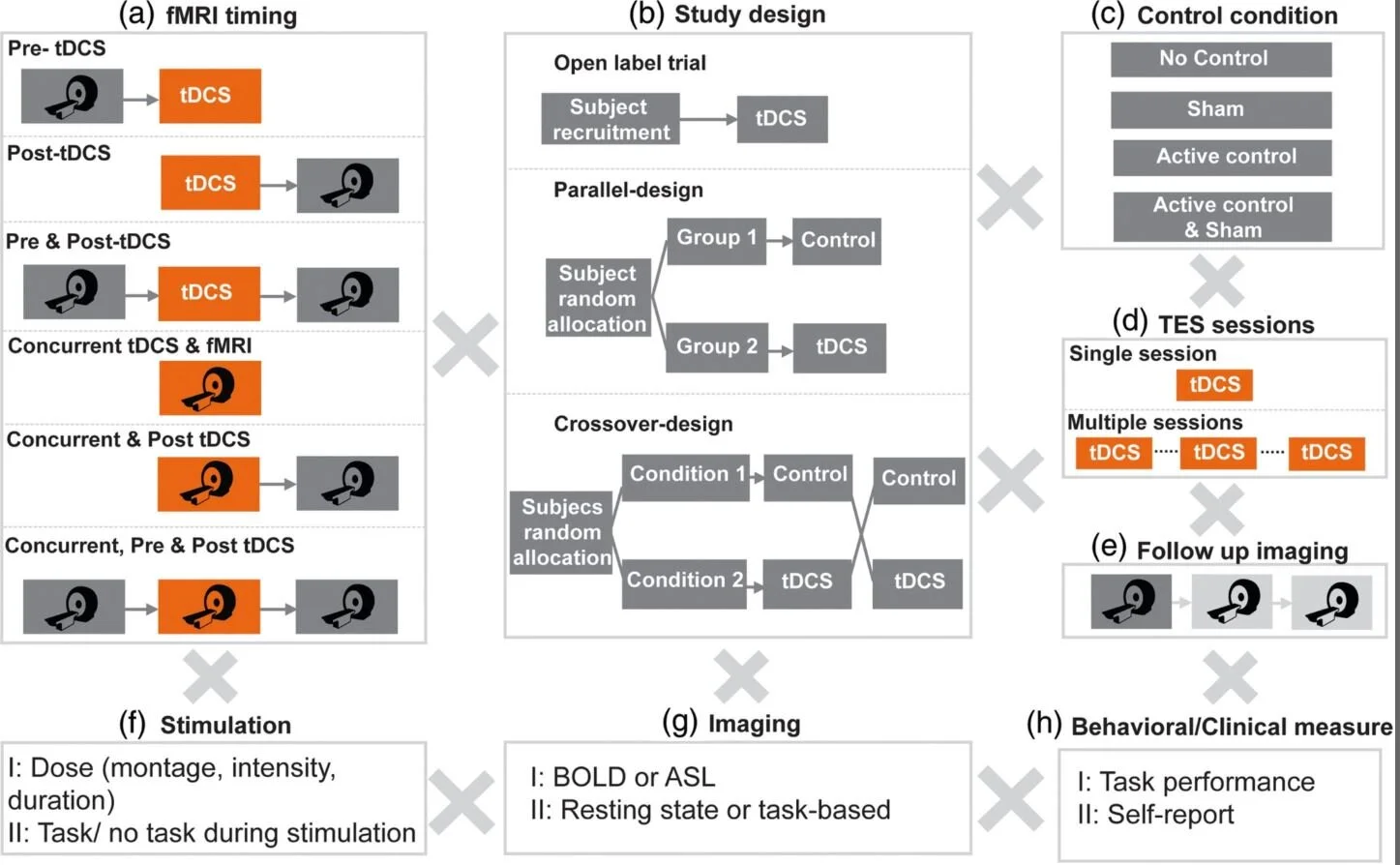
Understanding and reducing variability of response to transcranial direct current stimulation (tDCS) requires measuring what factors predetermine sensitivity to tDCS and tracking individual response to tDCS. Human trials, animal models, and computational models suggest structural traits and functional states of neural systems are the major sources of this variance. There are 118 published tDCS studies (up to October 1, 2018) that used fMRI as a proxy measure of neural activation to answer mechanistic, predictive, and localization questions about how brain activity is modulated by tDCS. FMRI can potentially contribute as: a measure of cognitive state‐level variance in baseline brain activation before tDCS; inform the design of stimulation montages that aim to target functional networks during specific tasks; and act as an outcome measure of functional response to tDCS. In this systematic review, we explore methodological parameter space of tDCS integration with fMRI spanning: (a) fMRI timing relative to tDCS (pre, post, concurrent); (b) study design (parallel, crossover); (c) control condition (sham, active control); (d) number of tDCS sessions; (e) number of follow up scans; (f) stimulation dose and combination with task; (g) functional imaging sequence (BOLD, ASL, resting); and (h) additional behavioral (cognitive, clinical) or quantitative (neurophysiological, biomarker) measurements. Existing tDCS‐fMRI literature shows little replication across these permutations; few studies used comparable study designs. Here, we use a representative sample study with both task and resting state fMRI before and after tDCS in a crossover design to discuss methodological confounds. We further outline how computational models of current flow should be combined with imaging data to understand sources of variability. Through the representative sample study, we demonstrate how modeling and imaging methodology can be integrated for individualized analysis. Finally, we discuss the importance of conducting tDCS‐fMRI with stimulation equipment certified as safe to use inside the MR scanner, and of correcting for image artifacts caused by tDCS. tDCS‐fMRI can address important questions on the functional mechanisms of tDCS action (e.g., target engagement) and has the potential to support enhancement of behavioral interventions, provided studies are designed rationally.
Vladimir V. Lazarev, Nigel Gebodh, Tiago Tamborino, Bikson, M, & Egas Caparelli-Daquer. (2020). Experimental-design Specific Changes in Spontaneous EEG and During Intermittent Photic Stimulation by High Definition Transcranial Direct Current Stimulation. Neuroscience, 426, 50–58. https://doi.org/10.1016/j.neuroscience.2019.11.016
Download PDF published in Journal Neuroscience Methods— DOI
Abstract
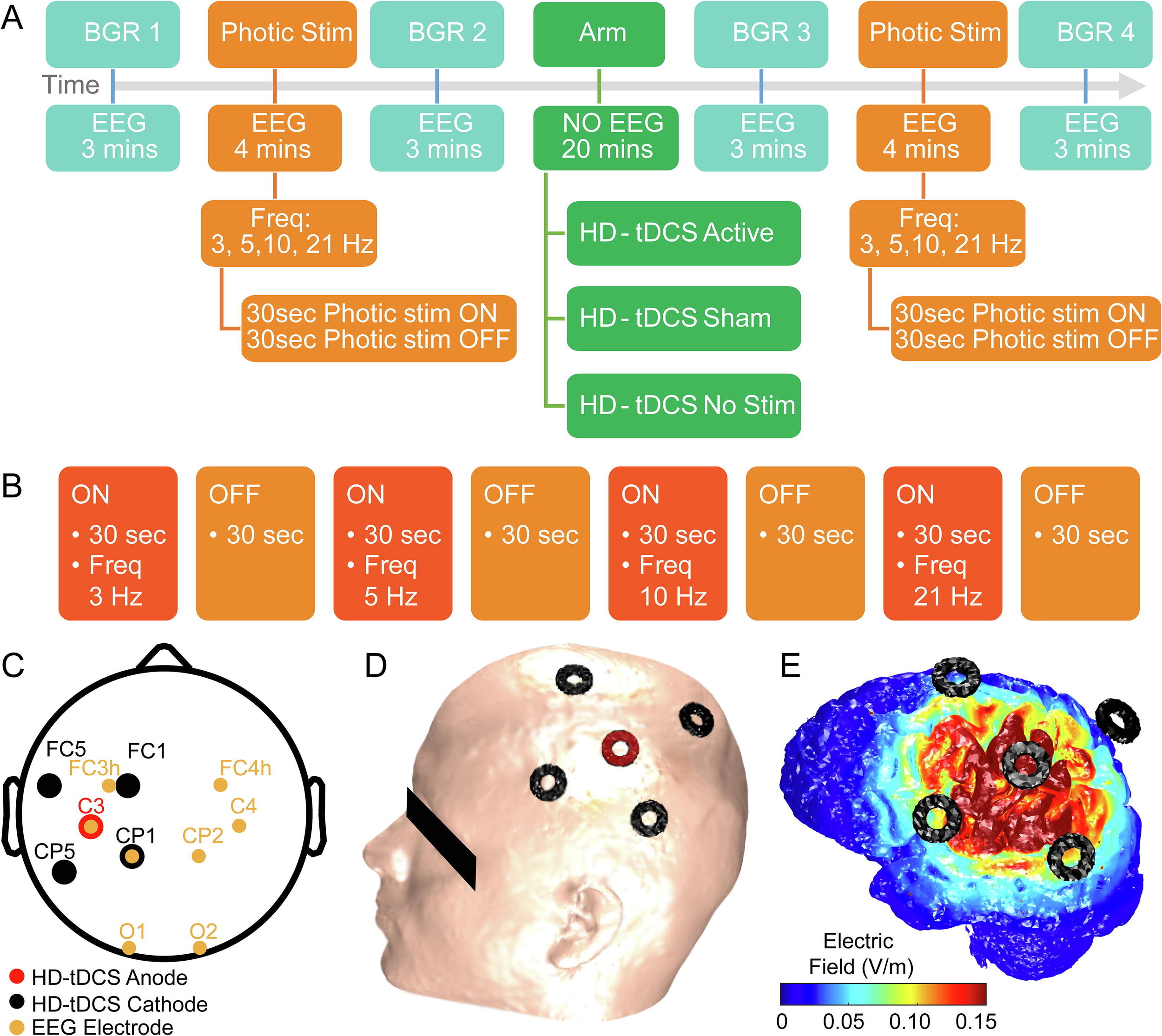
Electroencephalography (EEG) as a biomarker of neuromodulation by High Definition transcranial Direct Current Stimulation (HD-tDCS) offers promise as both techniques are deployable and can be integrated into a single head-gear. The present research addresses experimental design for separating focal EEG effect of HD-tDCS in the ‘4-cathode × 1-anode’ (4 × 1) montage over the left motor area (C3). We assessed change in offline EEG at the homologous central (C3, C4), and occipital (O1, O2) locations. Interhemispheric asymmetry was accessed for background EEG at standard frequency bands; and for the intermittent photic stimulation (IPS). EEG was compared post- vs pre-intervention in three HD-tDCS arms: Active (2 mA), Sham (ramp up/down at the start and end), and No-Stimulation (device was not powered), each intervention lasting 20 min. The asymmetric background EEG changes were only in the central areas with right-side amplitude spectra prevalence, most pronounced in the no-stimulation arm, where they depended on comparison time-points and were consistent with markers of transition between drowsiness and vigilance – bilateral decrease in the delta and asymmetric central increase in the alpha and beta1 bands. For the active arm, similar but less pronounced changes occurred in the alpha band. In contrast, responses to IPS developed similar asymmetric amplitude increase at four harmonics of the IPS of 3 Hz only in the active arm, against a background of a brain-wide symmetric increase in both active and sham arms. Our protocols and analyses suggest methodological caveats for how EEG of tDCS studies could be conducted to isolate putative brain polarization outcomes.
Computational Finite Element Method (FEM) forward modeling workflow for transcranial Direct Current Stimulation (tDCS) current flow on MRI-derived head: Simpleware and COMSOL Multiphysics tutorial. Ole Seibt, Dennis Truong, Niranjan Khadka, Yu Huang, Marom Bikson. bioRxiv 704940; doi: https://doi.org/10.1101/704940
Download PDF from bioRxiv - DOI
Abstract
Transcranial Direct Current Stimulation (tDCS) dose designs are often based on computational Finite Element Method (FEM) forward modeling studies. These FEM models educate researchers about the resulting current flow (intensity and pattern) and so the resulting neurophysiological and behavioral changes based on tDCS dose (mA), resistivity of head tissues (e.g. skin, skull, CSF, brain), and head anatomy. Moreover, model support optimization of montage to target specific brain regions. Computational models are thus an ancillary tool used to inform the design, set-up and programming of tDCS devices, and investigate the role of parameters such as electrode assembly, current directionality, and polarity of tDCS in optimizing therapeutic interventions. Computational FEM modeling pipeline of tDCS initiates with segmentation of an exemplary magnetic resonance imaging (MRI) scan of a template head into multiple tissue compartments to develop a higher resolution (< 1 mm) MRI derived FEM model using Simpleware ScanIP. Next, electrode assembly (anode and cathode of variant dimension) is positioned over the brain target and meshed at different mesh densities. Finally, a volumetric mesh of the head with electrodes is imported in COMSOL and a quasistatic approximation (stead-state solution method) is implemented with boundary conditions such as inward normal current density (anode), ground (cathode), and electrically insulating remaining boundaries. A successfully solved FEM model is used to visualize the model prediction via different plots (streamlines, volume plot, arrow plot).
Valero-Cabré A, Sanches C, Godard J, Fracchia O, Dubois B, Levy R, Truong DQ, Bikson M, Teichmann M. (2019). Language boosting by transcranial stimulation in progressive supranuclear palsy. Neurology, 10.1212/WNL.0000000000007893. https://doi.org/10.1212/wnl.0000000000007893. PDF
Download: PDF published in Neurology – DOI
Abstract
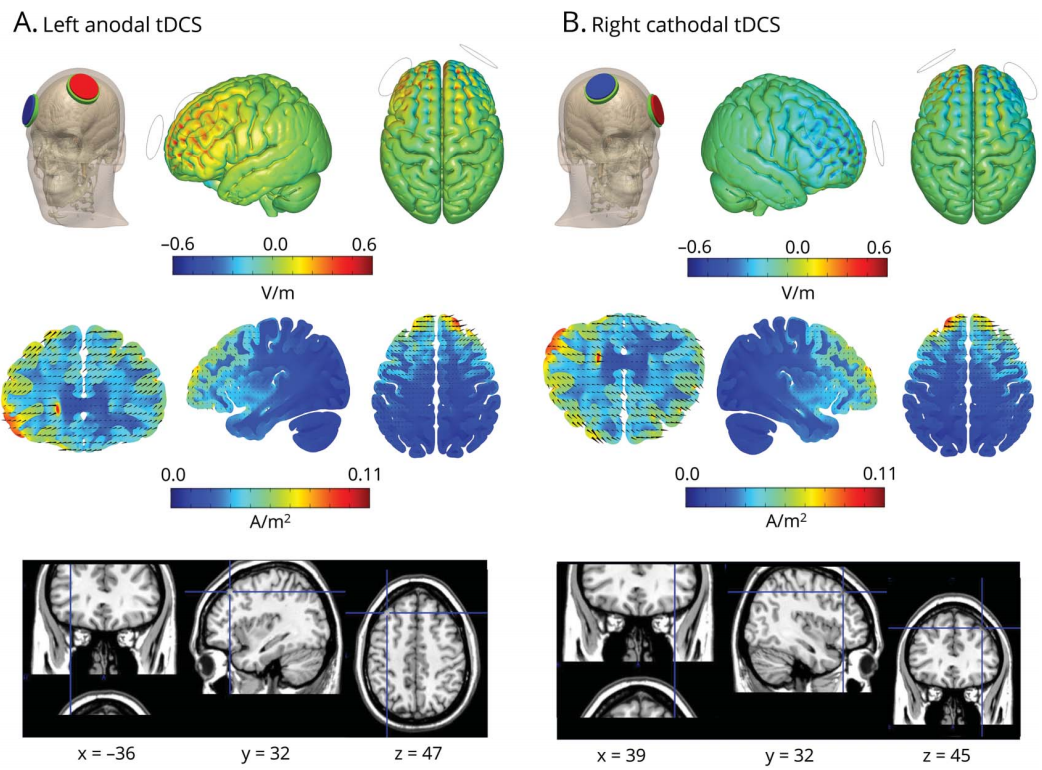
[Our objective was t]o explore whether transcranial direct current stimulation (tDCS) over the dorsolateral prefrontal cortex (DLPFC) can improve language capacities in patients with progressive supranuclear palsy (PSP). We used a sham-controlled double-blind crossover design to assess the efficiency of tDCS over the DLPFC in a cohort of 12 patients with PSP. In 3 separate sessions, we evaluated the ability to boost the left DLPFC via left-anodal (excitatory) and right-cathodal (inhibitory) tDCS, while comparing them to sham tDCS. Tasks assessing lexical access (letter fluency task) and semantic access (category judgment task) were applied immediately before and after the tDCS sessions to provide a marker of potential language modulation. The comparison with healthy controls showed that patients with PSP were impaired on both tasks at baseline. Contrasting poststimulation vs prestimulation performance across tDCS conditions revealed language improvement in the category judgment task following right-cathodal tDCS, and in the letter fluency task following left-anodal tDCS. A computational finite element model of current distribution corroborated the intended effect of left-anodal and right-cathodal tDCS on the targeted DLPFC. Our results demonstrate tDCS-driven language improvement in PSP. They provide proof-of-concept for the use of tDCS in PSP and set the stage for future multiday stimulation regimens, which might lead to longer-lasting therapeutic effects promoted by neuroplasticity. This study provides Class III evidence that for patients with PSP, tDCS over the DLPFC improves performance in some language tasks.